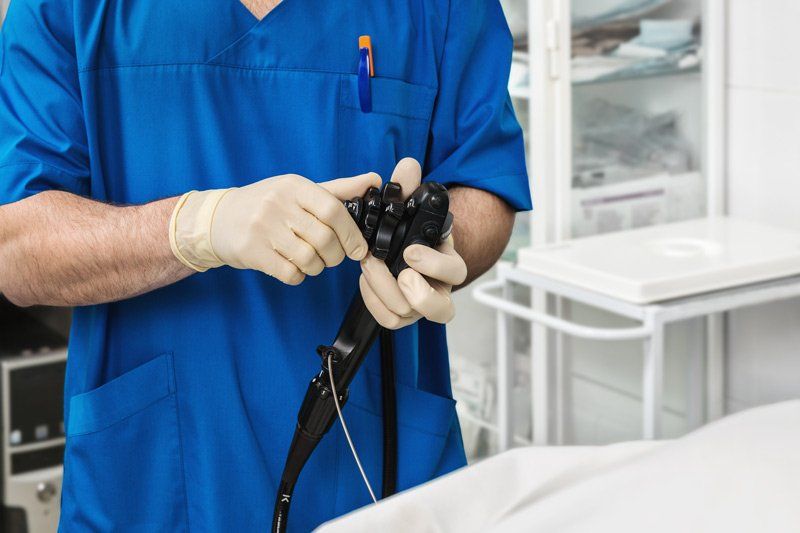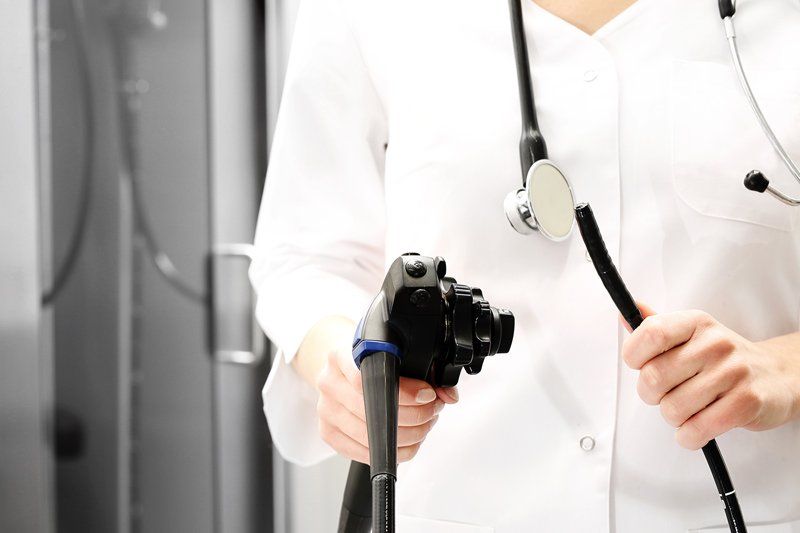
What Is a Colonoscopy?
A colonoscopy is a relatively safe and well-tolerated method of examining the large intestine or colon. This procedure has an advantage over radiological imaging, such as barium enemas or CT scans because it allows biopsies to be taken or polyps to be removed.
The colonoscope is a long and flexible tube about the thickness of your index finger. It is inserted through the rectum into the large intestine to allow inspection of the bowel. As cancer of the large bowel arises from pre-existing polyps (a benign, wart-like growth), it is advisable that any polyps found should be removed at the time of examination. Most polyps can be removed at the time of the procedure.
The Proper Preparation
Prior to the colonoscopy, you will be provided with a preparation kit containing full instructions. You should only ingest clear fluids the day before your procedure. On either the evening before or the morning of the procedure, you will need to drink a salty-tasting solution that completely cleanses the colon. Occasionally, this solution may cause nausea, vomiting and abdominal pains. Please phone your endoscopy unit if you have any symptoms that concern you.
As sedative drugs may be used during the procedure, it is essential for female patients to inform the nursing staff if there is any chance you might be pregnant. You should also advise them if you have heart valve disease, a pacemaker or are allergic to any drug or substance. Iron tablets or drugs to stop diarrhoea should not be taken for several days before your procedure. Please do not stop any blood thinners or anticoagulants unless directly advised to by your doctor.
What Is a Gastroscopy?
Gastroscopy is a safe method that it involves the use of a flexible tube to examine the upper intestinal tract. This includes the oesophagus, stomach and duodenum (upper small bowel). The procedure is commonly undertaken if your doctor suspects that you have inflammation of the oesophagus, an ulcer or another abnormality.
This examination is done following intravenous sedation. As a result, it is unlikely you will have any recollection of the procedure. It is extremely uncommon to have an allergy to the drugs used. Occasionally, it is necessary to perform interventional procedures through the endoscope, such as the removal of polyps from the upper intestine.
How to Prepare for It
While fasting, take all your regular medication with a sip of water. If you are diabetic, please contact your endoscopist to discuss this. The procedure will take between five and 15 minutes and you will be sleepy for about half an hour afterwards.

After Your Procedure
Gastrointestinal endoscopies are usually simple and safe. It is very unlikely to cause any serious problems. For colonoscopy patients, the sedative painkiller you are given before your procedure is very effective in reducing any discomfort. However, it may also affect your memory and you may find you are unable to recall details of your discussion with your doctor. For this reason, a relative or friend should come with you and you should contact your doctor for any necessary clarifications.
If you have any severe abdominal pain, bleeding from the back passage, fever or other symptoms that cause you concern, contact your doctor immediately.